The impact of the SARS-CoV-2 pandemic on Psychiatric Hospital Care Rehabilitation – A preliminar study

Italian version – English version
Introduction
At the Maria Luigia Hospital, we have a therapeutic protocol specifically designed for treating elderly patients with psychiatric or neurological issues accompanied by behavioral problems. The protocol includes the use of psychopharmacological drugs and participation in group therapies. However, to comply with the regulations governing social distancing after the SARS-CoV2 pandemic started in February 2020, we had to modify the rehabilitation program to be delivered in smaller groups with a reduced patient count, resulting in a reduced frequency of sessions. In addition, we had to temporarily suspend psychomotor activities that did not allow for the maintenance of social distancing.
We compared two cohorts, the pre-pandemic group (patients admitted in 2019) and the pandemic group (patients admitted in 2021). We found, unexpectedly compared to our hypotheses, a greater improvement in patients in 2021 in depressive symptoms measured with the Geriatric Depression Scale (GDS). Further investigations are planned to understand the factors that led to this difference.
Objective
This study aims to evaluate the prevalence and severity of mood disorders in the target population in light of the literature on the effects of the pandemic on the geriatric population (Mueller et al., 2022, Skoog et al., 2020). In addition, the study will also assess any differences in clinical outcomes in the pre-pandemic period (2019) and the pandemic period (2021).
Materials and Methods
2 cohorts of psychogeriatric inpatients were selected, admitting in 2019 (N=202) and 2021 (N=187). Differences between groups were evaluated according to socio-demographic variables (age, sex, civil status), scores at admission tests (GDS, MMSE, and Barthel Index), and participation frequency, through ANOVA and chi-square analyses. We also evaluated differences in clinical outcomes between the two groups of inpatients by narrowing the sample according to the following inclusion criteria:
a) to undergo an ordinary hospitalization (between 4 and 8 weeks)
b) to have participated in at least 40% of the groups
Data were analyzed through R version 4.2.0.
Results
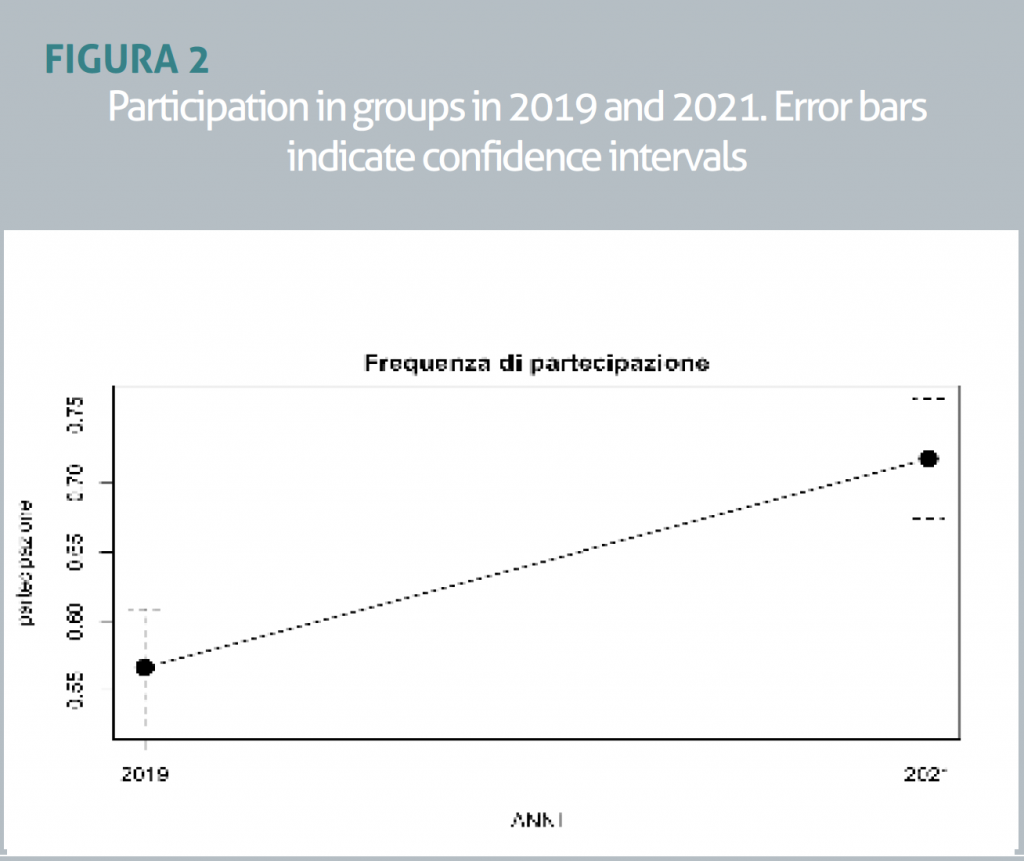
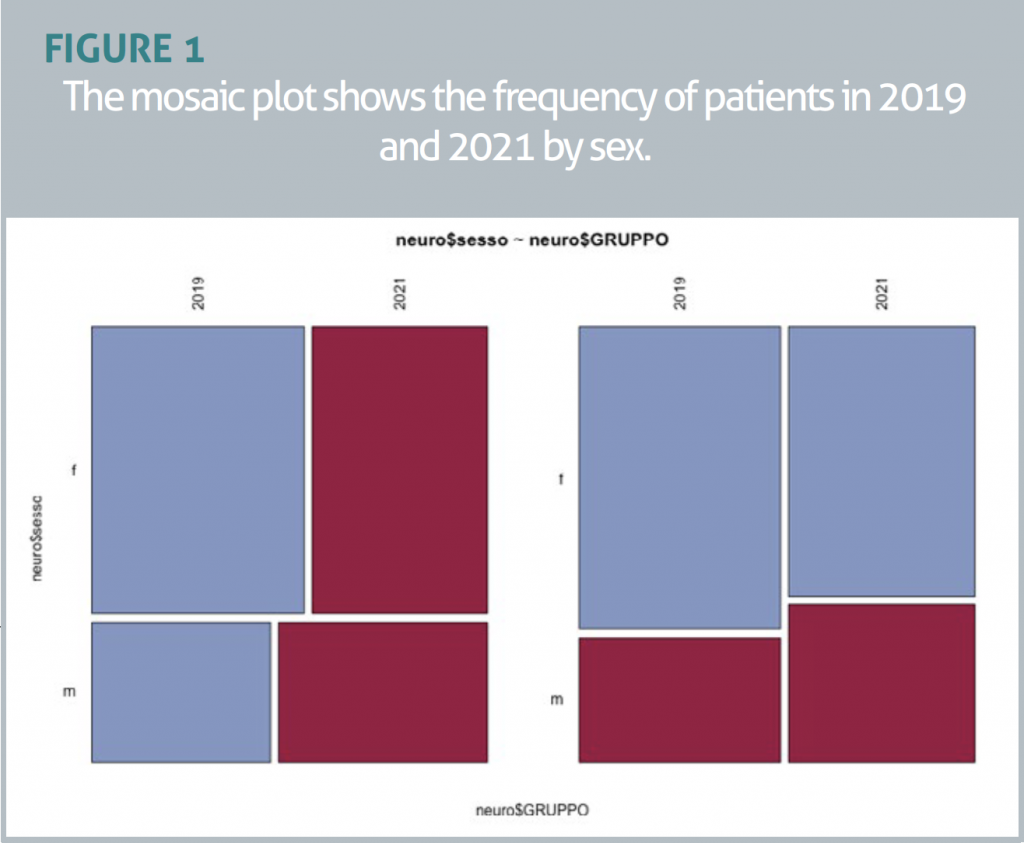
We found that the proportion of males and females did not differ between the two groups (OR=0.89; CI = 0.681 – 1.033), but the intragroup difference was significant, with a majority of female patients in both cohorts (FIGURE 1). Although the mean age was different in the two groups, from 73.52 in 2019 to 71.79 in 2021, this difference was not statistically significant (t=-1.63, p=0.103). There were no differences between the two groups in the T0 scores for MMSE (t= 0.39, p=0.69), GDS (t=-0.78, p=0.43) and Barthel Index (t= -0.84, p=0.40). There was a significant difference in the frequency of participation in groups (groups attended/groups planned), which increased from m=0.56 in 2019 to m=0.71 in 2021 (t= 4.913, p<0.001, F=24.14) (FIGURE 2).
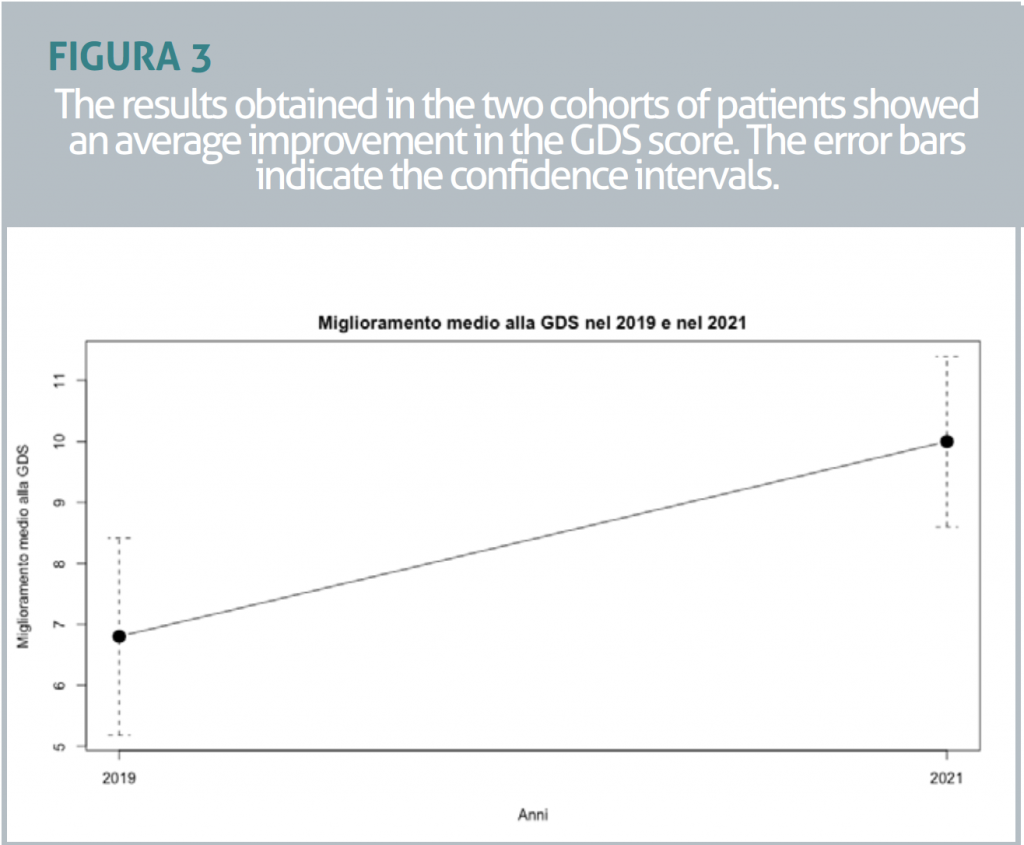
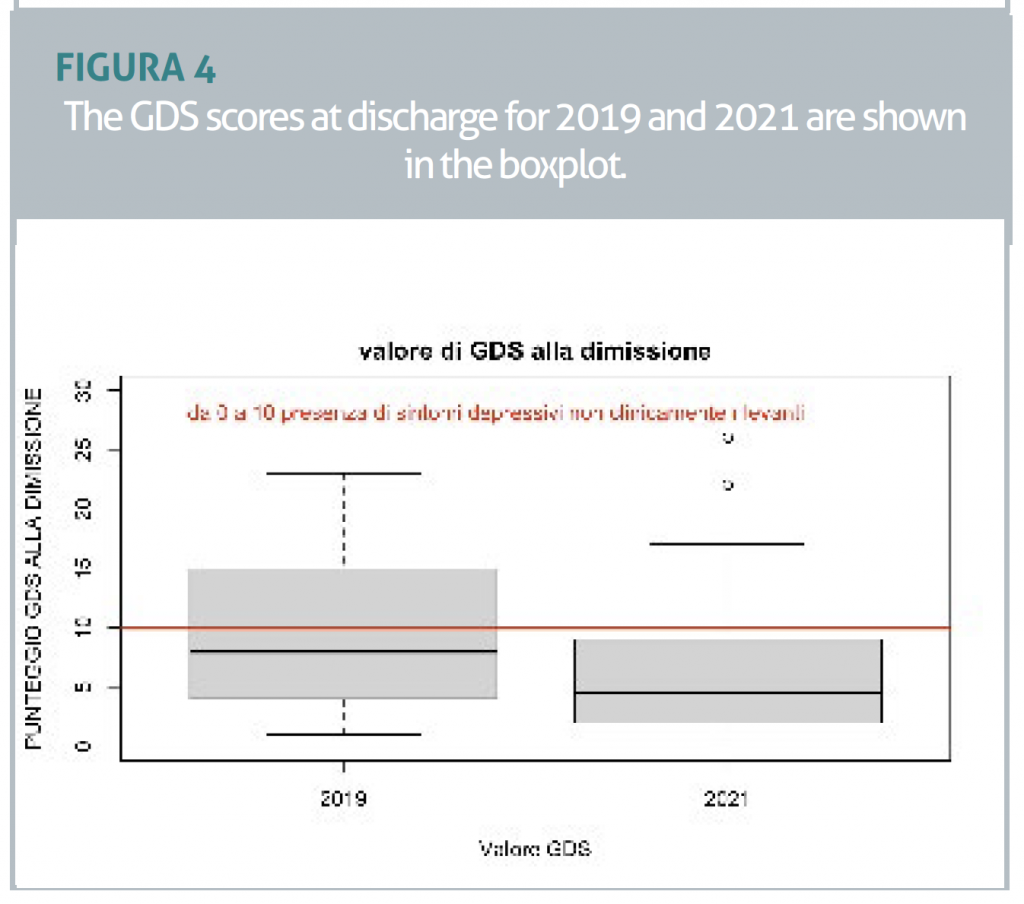
We therefore restricted the sample to those meeting the inclusion criteria (N=149) and continued the analysis. We found no significant differences between the two groups in the mean improvement on the MMSE (t=0.69, p=0.49) or the Barthel Index (t=0.019, p=0.98). The difference in the mean improvement on the GDS was significant between the two groups (t=8.96, p=0.0034, F=8,819). The group in 2021 showed a mean improvement of 3.37 points higher than in 2019 (FIGURE 3 and FIGURE 4). Finally, looking only at the 2021 sample, the means of those who had also had individual sessions with a psychologist or physiotherapy sessions in addition to group activity were not significantly different and did not explain the observed effect (FKT, t=-0.32, p=0.75; PSICO t=0.793, p=0.43).
Discussion and conclusion
Our preliminary study aimed to analyze whether the SARS-Covid2 pandemic had influenced the prevalence and severity of psychiatric symptoms in the population of geriatric patients hospitalized at the Maria Luigia Hospital. Subsequently, we evaluated whether the changes to the rehabilitation protocol had influenced the treatment outcomes. Our data suggest that the number of patients treated in the department has not changed when considering clinical variables (GDS, MMSE, and BARTHEL at T0) and sociodemographic variables. Furthermore, although the age difference is not statistically significant, the average age of patients hospitalized has decreased, possibly as a result of increased demand for health in the geriatric field, as already documented in the literature (Mueller et al., 2022; Broadbent et al., 2021; Bhome et al., 2021, Van der Velpen et al., 2021).
The improvement in outcomes at T1, observed with the GDS scores, is unexpected compared to the expected hypothesis, that is, that the modification to the protocol caused a worsening or, at best, an equivalence in clinical outcomes. However, a broader collection of data with a more focused analysis of clinical records is planned to deepen the observed effect. At the moment, we can formulate some hypotheses:
a) the participation in groups with a limited number of patients could have increased the effectiveness of the treatment by favoring prosocial dynamics (Hwang et al., 2020, Liu et al., 2016), despite the reduction in the number of patients for each patient.
b) the stay in a locked ward, without access to common areas, the suspension of visits by relatives inside the department, and the exit permits could have positively influenced patients’ motivation and active participation in the groups.
In conclusion, the suspension of psychomotor activities does not seem to harm the outcomes of rehabilitation
Compliance with Ethical Standards:
Conflict of Interest: All the authors declare no conflict of interest.
Ethical approval: All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. The study is approved by Ethics Committee of Area Vasta Emilia Nord (Prot. 19450; 05/06/2022)
Printed in: Conference Proceeding National Conference 2022, Florence
Authors:
- Artoni Paolo 1,3
- De Bernardis Elena1
- Foroni Francesca1
- Turrini Giuliano 1
- Pingani Luca 2
- De Bernardis Marco1,2
affiliation
- “Maria Luigia” Hospital – via Montepelato Nord, 41 – 43022 Monticelli Terme, Parma (Italy), ospedalemarialuigia.it
- Università degli studi di Modena e Reggio Emilia
- Corresponding author – artoni@ospedalemarialuigia.it – https://orcid.org/0000-0002-9275-9772
DOI: 10.13140/RG.2.2.33180.56965 – PDF AVAILABLE
References
• Artoni, P., et aL.,(2017). Depressione nell’anziano: studio di efficacia sul trattamento proposto dall’Ospedale Maria Luigia. AIP Congress Proceedings, (April), 2–3. https://doi.org/10.13140/RG.2.2.20968.60168
• Broadbent, et al., (2021). Mortality among mental health services for older adults during the COVID-19 pandemic: A retrospective analysis from South London. International Psychogeriatrics, 33(5), 527–528. https://doi.org/10.1017/S1041610221000442
• De Bernardis, M. et al., (2016). Studio pilota sull ’ efficacia di un trattamento terapeutico- riabilitativo integrato nel reparto di neuropsicogeriatria dell ’ ospedale “ Maria Luigia ” di Monticelli Terme ( PR ). AIP Congress Proceedings, (October 2021). https://doi.org/10.13140/RG.2.2.13454.48962
• Hwang, et al., (2020). Loneliness and social isolation during the COVID-19 pandemic. International Psychogeriatrics, 32(10), 1217–1220. https://doi.org/10.1017/S1041610220000988
• Liu, et al., (2016). Social support mediates loneliness and depression in elderly people. Journal of Health Psychology, 21(5), 750–758. https://doi.org/10.1177/1359105314536941
• Mueller, C., et al., (2022). A retrospective analysis of patient flow in mental health services for older adults in South London during the COVID-19 pandemic. International Psychogeriatrics, 1–2. https://doi.org/10.1017/S1041610221002775
• Skoog, I. (2020). COVID-19 and mental health among older people in Sweden. International Psychogeriatrics, 32(10), 1173–1175. https://doi.org/10.1017/S104161022000143X
• Van der Velpen, et al., (2022). Determinants of social health trajectories during the COVID-19 pandemic in older adults: the Rotterdam Study. International Psychogeriatrics, 1–15. https://doi.org/10.1017/S1041610221002891